How the COVID-19 pandemic is proving it’s crucial to improve health systems
A year after the world’s largest vaccine supply operation began, here’s what needs to happen next.

One year ago, a historic batch of COVID-19 vaccines arrived in Ghana. That batch was the first of its kind through the COVAX initiative – a ground-breaking global collaboration, committed to the development, production and equitable distribution of vaccines around the world.
As the first shots reached the arms of Ghanaians, the country’s president, Nana Akufo-Addo, reflected on the moment: "COVID-19 has changed the world. It has cost lives, battered health systems, and damaged livelihoods,” he said. “But, through these challenges, we have seen the best of humanity exemplified through strong multilateral cooperation.”
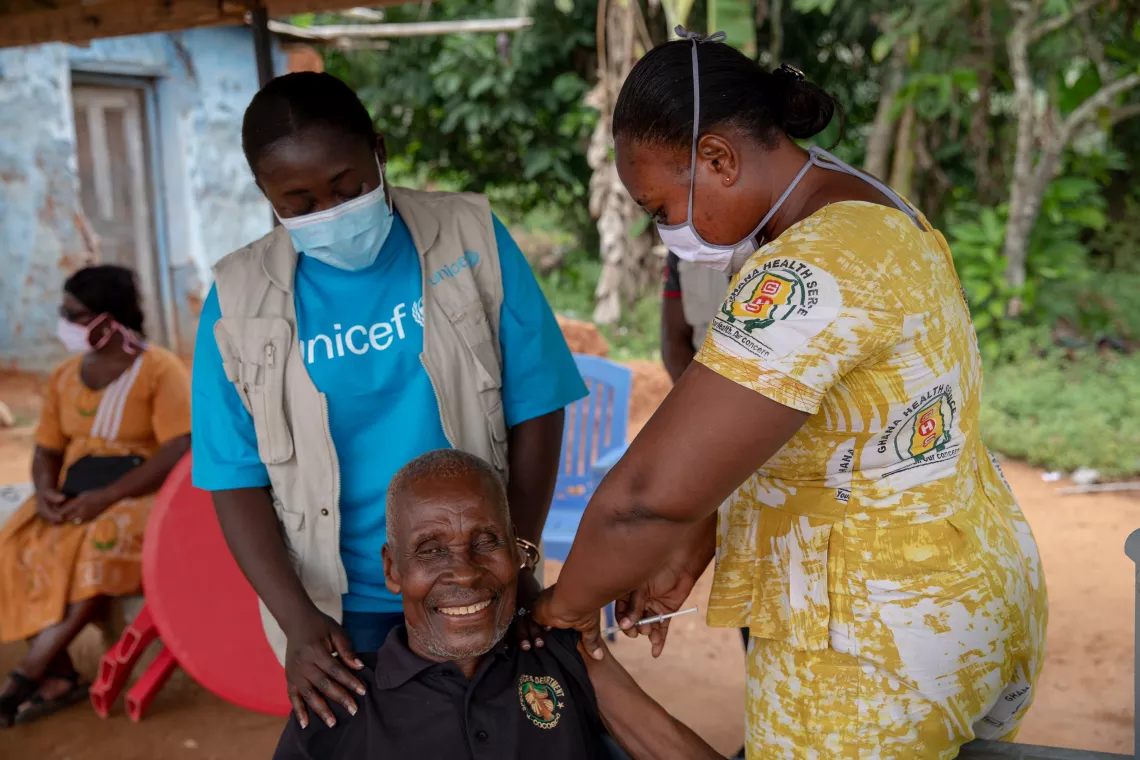
That multilateral cooperation has meant that the COVAX facility has become the largest vaccine supply operation ever. From crossing difficult terrain on foot in order to reach families in remote Nepalese villages to vaccinating elderly communities in Peru, the effort has been unprecedented.
For 83-year-old Artemio Baldoceda, who was one of those in Peru to receive the vaccine through COVAX, there was one simple thing that was top of mind when he found out he was going to get the shot:
“When I can hug my grandchildren tight, that moment is going to be glorious.”
Since COVAX was launched, more than a billion doses of the COVID-19 vaccine have been shared in more than 140 countries. The delivery of COVID-19 vaccines through this initiative is one of our greatest hopes of reducing the tragic loss of life and helping get the pandemic under control.

The COVAX facility is committed to global vaccine equity. And since late 2021, deliveries to low-income countries have been steadily increasing. Protecting those most-at-risk and health care workers in these countries is crucial to mitigating the public health and economic impact of the pandemic.
But one year since the delivery of that first batch of vaccines, hurdles still exist. Those hurdles are preventing countries from getting vaccines into people’s arms quickly and efficiently. As we mark this anniversary, it’s critical they’re acknowledged.
Focusing on the supply chain
What's the issue?
It’s essential that low-income countries are not only receiving vaccines, but also have the necessary financial resources to get hold of the other tools that are crucial to getting the doses get into arms. Think about all the syringes you need. The transportation that’s required. The ultra-cold chain freezers that store the vaccines. And then of course the funds needed to pay healthcare workers. Those financial resources have sometimes been scarce.
Then there’s the issue of vaccine waste. To be clear, wastage is normal and to be expected during any vaccination campaign, but there are a few things that can be done to limit the impact. COVAX is operating as a clearing house – channeling generous donations of doses to countries that can use them. But if doses are donated just a few weeks before their expiration date, that can lead to unintentional waste. That’s because the countries receiving the doses need enough time to put in place the logistics required to get those doses to arms.


What are some of the solutions?
When it comes to donating doses and limiting waste, it’s essential that the countries contributing vaccines only offer shots that have at least 10 weeks of shelf life left. That time allows for the necessary logistics and resources to be rolled-out, so the vaccines reach the communities that need them most.
Additionally, some countries are better prepared to receive and administer vaccines than others at certain times. So, it’s essential that donating countries avoid earmarking dose donations to specific countries. That means COVAX can allocate vaccines based on how prepared a country is at that specific time.
Clearly, the effective and efficient distribution of vaccines is pivotal to saving lives, tackling the pandemic and getting children back into school. But as we’ve mentioned, the actual vaccines are just one part of this challenge. Getting the dose into somebody’s arm requires a healthcare worker. It requires cold storage. Then there are the syringes and the protective equipment that’s required. In short, it requires an entire health system.
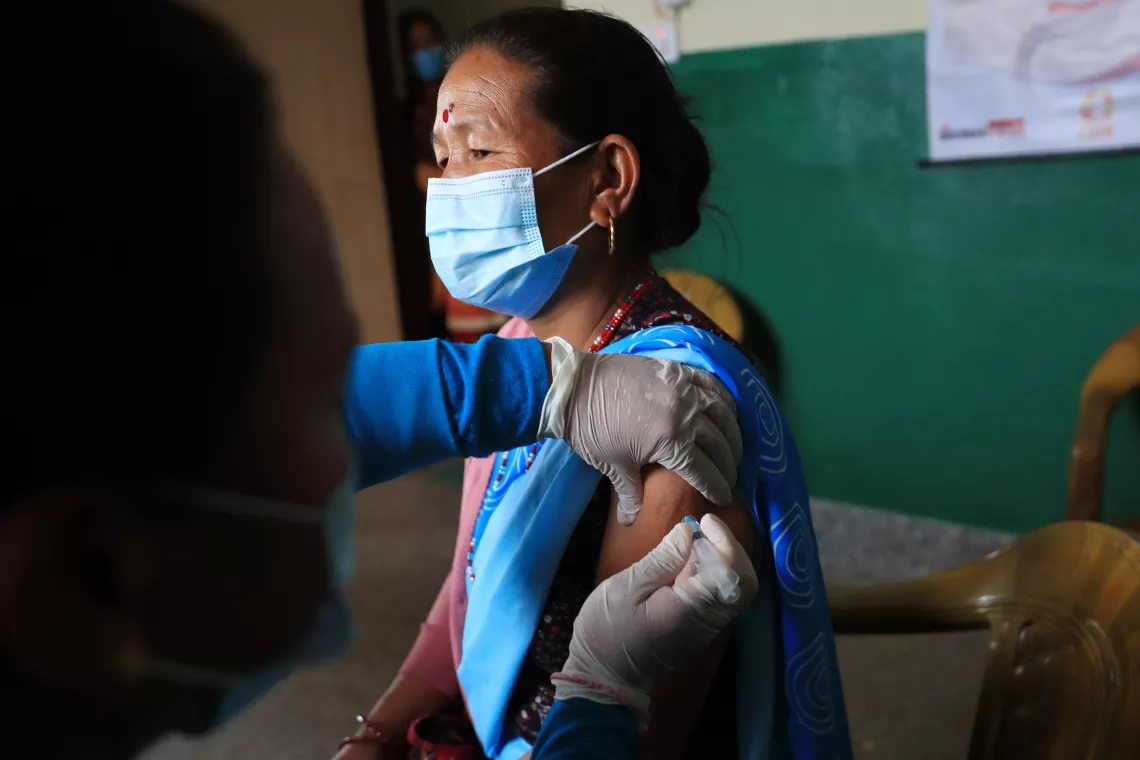
Improving health systems
We’ve spoken about the key supply and procurement issues that need to be addressed in 2022 to make sure that vaccines get to where they’re needed. But getting COVID-19 vaccines to people in low-income countries doesn’t just mean sending the doses. In every country, you need:
- An increased number of trained healthcare workers, like doctors and nurses, to administer vaccines
- An effective communication effort to let people know what the vaccine does, how it’s safe and why it’s so important for them and their communities
- Cold storage to get these temperature sensitive products to remote villages and a safe way to dispose of the syringes after the dose is given
- More vaccination sites, especially in rural communities, and pop-up vaccination sites in busy place like markets and bus stations
- Robust electronic health records, so it’s easy to figure out which communities have high or low vaccination rates to inform roll-out plans.


A strengthened health system, that includes those resources and that technology, requires significant financial investment moving forward. It’s paramount that funding from donors and international financial institutions is flexible and sustainable, so it doesn’t burden governments in the long run. And it’s crucial that any pandemic related funding doesn’t divert resources away from other essential healthcare services.
The pandemic has made it clear that improved health systems are paramount to not only getting everyone vaccinated and ending this pandemic, but better protecting people from health emergencies in the future and preventing future pandemics.
This is a crucial moment. A moment where if we recognize the value of investing in sustainable and fair health systems, there’s an opportunity to bring better health to more children and families than ever before.
Through the COVAX Facility – together with Gavi, the Vaccine Alliance, WHO and CEPI – UNICEF is leading efforts to procure and supply COVID-19 vaccines.




