UNICEF responds to seasonal uptick in acute respiratory infections in Afghanistan.
.


Ten-month-old Abbas is crying in his grandmother's lap, with tears rolling down his face over his parched lips. His grandmother, Fatema, adjusts his nasal tube but fails to comfort him. Abbas has pneumonia. He is one of 20 children being treated for acute respiratory infections (ARI) at the Sorabhi District Hospital Kabul Province, around 70 kilometres east of the capital.
Severe winter weather conditions, with temperatures well below zero in most of the country, lead to a sharp rise in the rate of acute respiratory infections every year. More than 160,000 ARI cases were reported in January 2024 across Afghanistan – a rise of about sixteen percent in comparison with the same time last year, largely due to severe weather conditions and air pollution. Children under five make up 62 per cent of the total number of cases.
Before bringing Abbas to the hospital four days ago, his family had tried to treat him using home remedies and cough syrup, but his health continued to decline. In the bitter cold of an Afghan Winter, Fatema walked for an hour along rough roads to reach the hospital. Once she arrived at Sorabhi District Hospital, doctors promptly diagnosed Abbas with pneumonia, and admitted him for treatment.
“Abbas has been sick for over ten days now. He has a fever, cough, and difficulty breathing. Since he was admitted to hospital, he has improved slowly,” says Fatema.
“The winter brings added burdens for us. We struggle to heat our home and keep our children warm. My other two grandchildren are also sick at home,” adds Fatema.
In an overcrowded outpatient ward at Sorabhi District Hospital, Dr Jan Agha is attending to sick children amidst cries echoing throughout the waiting area. It is 9:30 am, and he has already attended more than 20 sick children, with many more awaiting his care. Last week, Dr Agha treated 120 children – two or three times the usual weekly numbers - 80 per cent of whom were diagnosed with acute respiratory infections. While 30 of them are still receiving treatment for pneumonia in inpatient wards, the most severe cases were referred to a specialized children’s hospital in Kabul.
Dr. Agha attributes the rising number of respiratory infections not only to severe weather conditions but also to factors such as poverty, air pollution, inadequate respiratory hygiene, and overcrowded living conditions. The surge in ARI cases exacerbates the strain on already limited critical health care services, resulting in delayed treatment and increasing the risk of complications.
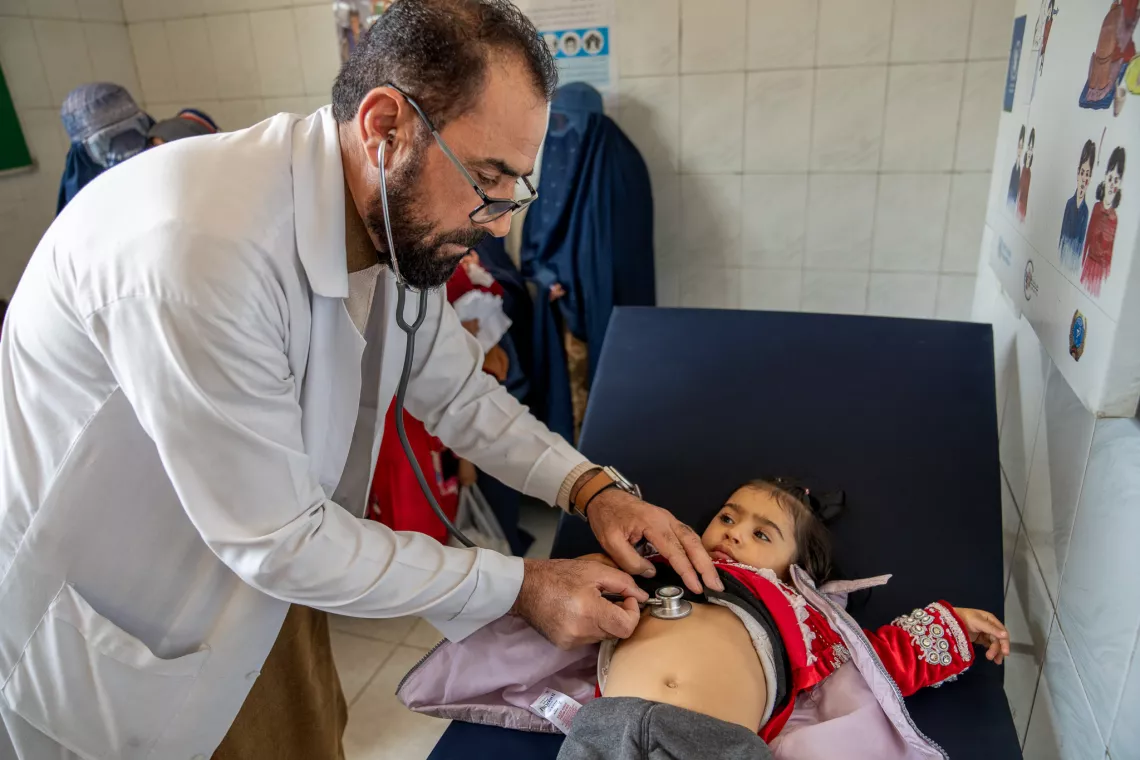
“Mothers come to our hospital bringing children with fever, coughs and pneumonia. As many Afghans slide into poverty, they find it increasingly difficult to afford adequate heating, causing the rate of respiratory infections to rise, especially among children and the elderly,” explains Dr Agha.
To cope with the rising number of cases, UNICEF, with support from the World Bank, prepositioned medical supplies and heating materials in health facilities to ensure prompt medical attention for the people affected. Across Afghanistan, in partnership with the World Bank and the Asian Development Bank, UNICEF plays a critical role in supporting the operational costs of around 2,400 health facilities and by covering the salaries of around 27,000 health workers, including that of Dr Agha. Last year, UNICEF's support for health workers like Dr Agha contributed to nearly 20 million children and their families receiving essential health and nutrition services.




